Shakahola Forest, Kilifi County, where over 400 lives were lost under the extremist teachings of Pastor Paul Mackenzie. Families still seek answers, as well as psychological and economic support, despite promises made by the government more than three years ago.
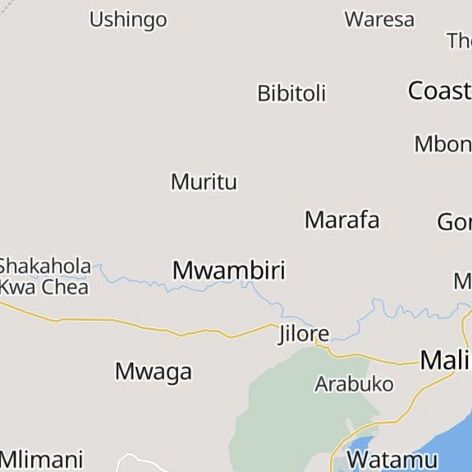
Map of Shakahola, Source: Kenyan Maps
Known as the Shakahola Forest incident, the massacre in Kilifi County, where more than 400 people were starved to death under the teachings of Pastor Paul Mackenzie, remains one of Kenya’s darkest recent tragedies, according to whistleblower Francis Wanje. Mackenzie instructed his followers to starve themselves in order to “meet Jesus,” a directive that led to mass deaths and the burial of victims in shallow graves.
Recent discoveries of bodies in nearby Kwa Binzaro have reignited fears that the network of harm may extend further. Directorate of Criminal Investigations linked the graves found there to the Shakahola tragedy, and exhumations continue amid calls for expedited forensic work and DNA identification. Local organizations, whistle-blowers, and human-rights advocates argue that earlier warning signs were ignored by authorities, allowing the cult to operate unchecked and expand deeper into rural areas.
Three years after the Shakahola tragedy, the wounds of loss have hardly healed. Fresh shallow graves discovered at Kwa Binzaro in May 2025 have reopened old traumas and exposed glaring gaps in accountability and oversight. Families in Kwa Binzaro are demanding more than arrests: a full truth about what happened, identification of all victims, justice for families, exposure of the entire network, licensing and oversight of religious organizations, comprehensive DNA-based identifications, psychological and social support for survivors, and policies to prevent extremist religious groups from operating unchecked. The fight is not only for justice for the dead, but for prevention for the living.
In Shanzu, Francis Wanje, a well-known teacher and the Shakahola whistleblower, still lives in trauma as he waits for DNA results to identify his remaining family members before burial. According to Wanje, his case against Pastor Paul Mackenzie, the leader of the sect, was dismissed in court despite Mackenzie being held behind bars.

Francis Wanje, the Shakahola whistleblower, awaits DNA results to identify his remaining family members. He clings to agriculture and teaching to give him hope for the loss. Photo Courtesy Teryani Mwadzaya
Wanje witnessed the horrors firsthand and fought for justice. Despite the arrests, his case against Mackenzie was dismissed. The trauma of loss lingers, compounded by bureaucratic delays in DNA identification.
“After I had informed the police about the tragedy, I left everything in the hands of the police, and I went to Chiromo Mental Health for two weeks as I was so exhausted seeing dead bodies in the forest,” Wanje said. “Last year, I got a call from the Directorate of Criminal Investigations, Malindi Police Station, informing me that four bodies of my family had been positively identified through DNA. We now await three more.”
Stanley Kahindi Karaga, who lost five members of his family, said that while some remains were identified and buried, no postmortem have been done to determine the causes of death, leaving many questions unanswered. “If we are to heal, then the truth should be released, and people should be counseled to accept what transpired,” Karaga explained.
In the villages, motorcycle riders, famously known as boda boda riders, have even acted as local investigators. Emmanuel Kenga said that seven riders who volunteered to search the forest were attacked, their motorcycles burned, and one was seriously injured. Choosing to volunteer was the hardest choice as many young men attempted, but they couldn’t do it yet, the act has since made Emmanuel Kenga shift work opportunity as he now experiences stigma from his clients naming him dirty and uncouth as he dug out dead bodies.

Emmanuel Kenga, a former boda boda rider, checks his maize farm in Shakahola. Photo Courtesy Teryani Mwadzaya.
Emmanuel Kenga risked life and limb volunteering to dig out graves, only to face attacks and social stigma. The bravery of boda boda drivers highlights the gaps in official response and community resilience as they volunteered to dig out the buried bodies in the forest. Kenya expressed his shock and trauma as he recalled seeing at least five to 12 bodies in one grave.
Till now, many Kenyans thought all the people in Shakahola died in the massacre, but it was not like that. Shakahola is very far away from the forest, and it is a trading Centre. It’s been more than a year and a half, and the community still hasn't been able to get any counseling, although they need it.

Shukrani Karisa Mangi and Emmanuel Kenga, part of the volunteer team that exhumed dead bodies in Shakahola Forest and Kwa Binzaro Forest. Photo Courtesy Teryani Mwadzaya.
Volunteers who exhumed dead bodies in Shakahola narrate their experience, still in grief, and decry psychological and economic support.
Simon Mwashighadi, the founder of the Voice of the Voiceless organization in Kilifi County, says the Shakahola massacre might have unfolded very differently if authorities had acted on the early warnings. Families of missing followers, local whistle-blowers, and even some junior officers had raised concerns months before the first graves were discovered, reporting strange disappearances and claims that Pastor Paul Mackenzie was urging his followers into extreme fasting.
“Religious leaders should be guided by the Constitution so they do not make people vulnerable,” Mwashighadi said, arguing that the tragedy exposed the fragile balance between protecting freedom of worship and enforcing safeguards against exploitation. His warning sits at the center of the ongoing national debate: how to ensure faith remains a source of refuge without becoming a shield for abuse.
Chairman of the Supreme Council of Kenya Muslims in Kilifi County, Sheikh Haroun Musa, added that people should be counseled and frequent talks should be given to the society. “The government failed to check the Shakahola incident in time, but society also needs to be educated on religious matters according to the religious beliefs they follow, so as not to be manipulated. Explained Sheikh Musa.
In Kwale, traditional healer Mupa Nyawa Chiboga treats patients with physical and emotional pain, but warned that some rogue preachers and self-proclaimed prophets secretly draw on black magic practices to tighten their grip on followers. Chiboga explained that rituals, potions, and psychological manipulation, locally referred to as Fungaliza, are used to create the illusion of supernatural authority and blind followers into submission.

Mupa Nyawa Chiboga, a traditional healer prepares medicine for her clients. Photo Courtesy Teryani Mwadzaya.
Mupa treats physical and emotional pain, warning against manipulative preachers who exploit superstition and black magic practices. Some rogue faith leaders manipulate spiritual beliefs for control. Responsible traditional healers, she argues, offer culturally trusted, regulated care, a balance that Kenya is now seeking to formalize.
“People think it is faith, but some of these potions are meant to confuse, weaken judgment, and make followers surrender their possessions or even abandon their families,” Mupa said.
The World Health Organization (WHO) recognizes that traditional, complementary, and integrative medicine plays a significant role in health systems worldwide and promotes its integration in evidence-based, regulated ways to ensure safe and quality healthcare.
The WHO has described a global strategy toward traditional and complementary medicine that aims to strengthen the evidence base, support safe practice through regulation, and integrate effective traditional care into national health systems.
Many people in low- and middle-income countries depend on traditional healers for healthcare needs, often due to cost, distance, mistrust of formal healthcare, or beliefs that modern medicine cannot address spiritual causes. This reliance highlights the need to balance cultural trust with evidence-based safety and regulation.
Gona Charo Kalama, a Shakahola resident, said that the government did not act in time when information was sent earlier, and people's lives could have been saved if information had been acted upon in time.
“I am so bitter since I tried to inform the chief and other authorities way back in 2019 till 2022. I was a farmer, and since I was an upcoming politician, I used to get information about the people who were starving from herders and other farmers, and when I informed the authorities, nothing happened,” explained Kalama.
As grassroots leaders push for community education and counseling on religious and human rights issues, some initiatives offer alternative paths toward resilience and protection against exploitation. Community savings groups supported by the Five Talents Organisation have helped locals build economic security and reduce vulnerability to predatory lenders and miracle-selling preachers.
Early assessments from the programme show members starting vegetable kiosks, tailoring shops, and small livestock project ventures that have survived economic shocks because they are supported by group loans and business mentorship. While the initiative has not eliminated poverty, it has provided a layer of stability.

Emmanuel Chaka, Chairman Muungano Farmers Group in Mariakani, Kilifi County, showcasing how mushrooms are grown. Photo Courtesy Teryani Mwadzaya.
Economic empowerment initiatives offer alternatives to predatory preachers and miracle cures, fostering community resilience.
Five Talents Organisation projects provide economic security, reducing vulnerability to exploitation and helping communities regain control over their futures.
“The long-term hope is to scale the model further so that such groups become a first line of social protection, one that cuts across faiths and offers people a practical alternative to desperation,” said Officer Gloria.
The long-term hope also intersects with global health policy: The World Health Organization’s Global traditional medicine strategy 2025-2034 envisions people-centered traditional, complementary, and integrative medicine integrated into national health systems with regulatory oversight, safe practice standards, and community empowerment. Within this context, Kenya’s efforts to integrate traditional medicine into formal healthcare offer both opportunity and challenge: how to harness indigenous knowledge safely while protecting citizens from harmful practices.
As Kenya seeks to integrate traditional medicine with modern healthcare, it faces a complex balancing act: expanding access to care while ensuring safety, efficacy, and respect for indigenous knowledge. The Kenyan government unveiled an ambitious plan to integrate traditional medicine into the mainstream healthcare system by 2028, marking a major shift in healthcare delivery, regulation, and recognition of cultural heritage.
Speaking at the Second WHO Global Summit on Traditional, Complementary and Integrative Medicine (TCIM) in New Delhi, Health Cabinet Secretary Aden Duale said the strategy would establish a National Policy and a Department of Traditional Medicine to transform a largely informal practice into a regulated, evidence-based, and collaborative health sub-sector. The framework was anchored on safety, scientific rigor, innovation, and respect for indigenous knowledge, with constitutional safeguards for biodiversity and equitable benefit-sharing, as traditional practitioners were set to work alongside conventional medical professionals in public health facilities.
Under the proposed model, patients visiting health facilities were expected to consult both medical doctors and accredited traditional practitioners, with treatments documented in shared medical records to improve safety, transparency, and continuity of care. Central to the plan was a proposed Traditional Medicine and Medicinal Plant Bill, which was intended to regulate practitioners, protect consumers, ensure quality and safety standards, and safeguard indigenous intellectual property, alongside complementary legislative efforts such as the Kenya Medical Research Institute Bill 2025, which sought to strengthen research, clinical testing, and oversight of traditional remedies.
Kenya’s reform aligns with a broader push by the World Health Organization and its partners to strengthen the role of traditional medicine within national health systems. According to the World Health Organization, traditional, complementary, and integrative medicine refers to knowledge and practices rooted in cultural beliefs and used for health maintenance, prevention, diagnosis, and treatment of illnesses.
Across Africa, approaches vary. Countries like Cameroon and Madagascar have successfully embedded traditional medicine into national health systems through formal policies, regulatory frameworks, and practitioner collaboration, including registries for healers, treatment guidelines, and joint training programs. Meanwhile, nations such as Namibia struggle with poor documentation, weak administrative structures, limited public trust, and a lack of research, all of which hinder integration into formal healthcare. Common continental challenges include the absence of standardized regulation, insufficient clinical research, and risks of foreign exploitation of indigenous remedies.
Kenya’s current initiatives, such as proposed clinical trials, regulatory oversight, and partnerships with research institutes, reflect an effort to harness the benefits of traditional medicine safely, preserving cultural practices while protecting citizens from harm.
Faith and spiritual beliefs further complicate this landscape. Multiple studies in Kenya show that religious and spiritual convictions, often intertwined with traditional healing practices, influence health-seeking behavior, sometimes with life-threatening consequences.
A 2025 KEMRI study on supernatural causes documented that in Nairobi’s informal settlements, religious conviction and belief in spiritual healing can lead some patients to discontinue anti-retroviral therapy, putting lives at risk. Mental health studies in rural counties echo this trend, with families often consulting traditional or faith-based healers before engaging modern psychiatric care due to stigma, mistrust, or the belief that modern medicine cannot address spiritual causes.
“The challenge is not just to educate, but to understand why people trust traditional or faith healers over doctors,” says Dr. Jane Mwende, a public health researcher in Nairobi. She added, “Any intervention must respect culture while protecting lives.” For Kenya, the stakes are high. The country must navigate the delicate intersection of faith, tradition, and modern science, striving to integrate indigenous knowledge safely into formal healthcare while curbing unsafe practices. As policymakers and researchers push for evidence-based regulation and collaboration with traditional healers, the goal remains clear: to ensure that cultural trust does not come at the cost of human life.
For decades, Kenya’s traditional medicine sector has thrived in the shadows, trusted by millions yet largely unregulated, often dangerous, and invisible to policymakers. Now, Parliament is poised to change that. The Kenya Medical Research Institute (KEMRI) Bill, currently awaiting debate, seeks to formally integrate traditional and alternative medicine into Kenya’s healthcare system, placing KEMRI at the helm of regulation, research, and approval.

Dr. Amos Lewa in a laboratory checking herbs. Photo Courtesy Teryani Mwadzaya.
Kenya Medical Research Institute (KEMRI) aims to scientifically validate and regulate traditional medicines, bridging cultural trust with safety. The KEMRI Bill proposes clinical testing, biochemical analysis, and regulation of traditional remedies.
This integration seeks to prevent tragedies like Shakahola, where unverified health claims were weaponized by extremists If passed, the law would require that herbal and alternative remedies undergo rigorous biochemical, pharmacological, and clinical evaluation before they can be marketed.
A national database would document validated traditional knowledge, safeguarding it against biopiracy while preserving indigenous heritage. Practitioners could face fines or imprisonment for distributing untested products, false advertising, or unsafe concoctions. In essence, the bill aims to transform a largely informal, culturally entrenched system into a regulated, scientifically supervised component of national healthcare.

Mohammed Kitsao Kadenge, a herbalist concentrating on meditation while awaiting responses from the universe, speaks to him. Photo Courtesy Teryani Mwadzaya.
For many, the proposal is long overdue. Public health advocates argue that regulation could dramatically reduce the thousands of preventable deaths linked to unsafe herbal remedies every year. Supporters also see an opportunity to professionalize traditional healers, giving them access to training, standardized protocols, and legitimacy within the broader healthcare system. “This is recognition that traditional medicine is part of our culture,” says Dr. Jane Mwende, a Nairobi-based public health researcher. Adding that with proper oversight, it can complement modern medicine safely.
Yet not everyone is convinced. Critics warn that stringent clinical requirements could push small-scale healers, many operating in rural or informal settings, out of business or underground, limiting access for the communities that rely on them most. Some concerns standardizing remedies may strip them of cultural nuances, discarding effective treatments that do not fit neatly into Western scientific frameworks. Others worry that the law, if poorly implemented, could legitimize some remedies without adequate public education on their limitations, encouraging people to bypass urgent medical care in favor of herbal alternatives.
In the public sphere, reactions are mixed. Traditional healers, particularly those with larger client bases or urban practices, largely celebrate the move as validation and opportunity. Among medical professionals and scientists, optimism is tempered with caution: regulation is necessary, but implementation will determine whether it saves lives or inadvertently creates new risks. Community forums in counties like Uasin Gishu and Kisumu show growing support for integration, though many rural healers remain wary of bureaucratic oversight.
The law’s potential impact reaches beyond Kenya’s borders. Across Africa, countries like Cameroon and Madagascar have successfully integrated traditional medicine into their national health systems, creating regulatory frameworks, practitioner registries, and joint training programs. Others, like Namibia, continue to struggle with poor documentation, lack of trust, and limited research showing that integration is far from simple. Kenya’s approach, by combining regulation with research and cultural preservation, may offer a model if handled with sensitivity.
The KEMRI Bill represents a delicate balancing act: respecting centuries-old indigenous practices while protecting public health. Its passage could mark a turning point for Kenya’s health sector, but the outcome will depend on thoughtful implementation, community engagement, and ongoing oversight. For millions who rely on herbal remedies, the stakes are high. The challenge now is ensuring that culture, safety, and science move forward together without leaving anyone behind. The Kenya Medical Research Institute Bill states that “The government shall recognize and integrate traditional medicine in a manner that complements the conventional healthcare system.”
According to the Kenya Medical Research Institute, integration would happen in several ways: by allowing KEMRI to scientifically test herbal products; by creating quality and safety standards for remedies already in circulation; and by giving regulatory bodies the evidence they need to approve, reject or monitor treatments used by millions of Kenyans. Moreover, trained traditional health practitioners could eventually be registered, guided, and held accountable under national health policies, rather than operating informally and beyond oversight.
For communities, this approach aims to bridge two worlds: acknowledging the long-standing cultural reliance on herbal medicine while protecting people from harmful, counterfeit, or exaggerated claims. And in the backdrop of tragedies like Shakahola, where unverified healing promises were used to lure followers away from medical care, this integration becomes more than a bureaucratic reform. It is a safeguard. By grounding traditional medicine in science, standards, and supervision, the government hopes to reduce the space in which misinformation, miracle cures, and extremist teachings can thrive.
If passed, the new mandate for the Kenya Medical Research Institute (KEMRI) to conduct clinical and biochemical tests on traditional treatments may seem like a purely scientific reform, though it touches directly on the environment that allowed the Shakahola tragedy to unfold. At the heart of the massacre was not only spiritual manipulation, but also dangerous, unverified health claims and teachings that discouraged modern medicine, promised miraculous healing, and urged followers to abandon hospitals in favor of “faith-only” treatment or extreme fasting.
By introducing scientific scrutiny to herbal remedies and traditional treatments, KEMRI’s role becomes a crucial counterweight to the misinformation and pseudoscience that extremist religious leaders often use to cement control. Many such sects rely on claims of supernatural healing powers, “anointed” potions, or herbal cures that are neither tested nor regulated. Formal research and safety checks create a baseline of truth about what works, what doesn’t, and what is harmful, making it harder for manipulative leaders to exploit people’s health fears or sell unverified solutions as divine interventions.
KEMRI, with the Ministry of Health and research organizations, aims to create innovation environments for comprehensive case management and precision medicine evaluation. During the recent KEMRI Annual Scientific Health conference, diseases like cancer, diabetes, and autoimmune diseases were identified for personalized medicine approaches. President Ruto recently endorsed the Quality Healthcare and Patient Safety Bill for 2025, which seeks to transform the health sector and establish an independent Quality Healthcare and Patient Safety Authority. The Kenya Medical Research Institute Bill, 2025, introduced by Seme MP James Nyikal, would create legal oversight for traditional medicine practices long used by Kenyans but often lacking quality control.
The World Health Organization (WHO) estimates that over 5,000 Kenyans die annually due to unsafe or unregulated traditional remedies, a statistic that exposes the widening gap between community beliefs and formal healthcare systems. Yet, for many families, herbalists remain the first or last line of hope, especially when modern medicine feels out of reach due to cost, distance, mistrust, or chronic under-staffing in public hospitals.
A 2023 Ministry of Health survey found that nearly 70% of Kenyan households use some form of traditional medicine, often without accurate dosage, clinical trials, or regulation. In rural counties like Kilifi, Kwale, and Tana River, herbal practitioners operate openly, trusted as custodians of indigenous knowledge but often working outside formal oversight. This reliance on unverified treatments has allowed harmful concoctions, misdiagnoses , and delayed referrals to silently contribute to preventable deaths. At the same time, policymakers are torn between preserving cultural healing systems and curbing rising quackery, an unresolved tension at the heart of Kenya’s struggle to integrate tradition with safe, evidence-based care.
According to the World Health Organization global draft strategy on traditional medicine 2025- 2034 aims to support member states in designing and implementing national strategy plans that will ensure research and provide safety standards that will enable the use of traditional medicine to support people's health and well-being.
As Kenya seeks to integrate traditional medicine with modern healthcare, it faces a complex balancing act: expanding access to care while ensuring safety, efficacy, and respect for indigenous knowledge. Across Africa, approaches vary.
Countries like Cameroon and Madagascar have seen elements of traditional medicine recognized within national health systems as in Cameroon where traditional medicine has been formally acknowledged and proposed for integration into the health system to complement conventional services, reflecting efforts to valorize indigenous healing practices alongside biomedical care, and in Madagascar where herbal remedies such as COVID-Organics drew global attention and have been subject to research interest, highlighting both potential and controversies around evidence-based use of traditional therapies. Meanwhile, nations such as Namibia struggle with poor documentation, weak administrative structures, limited public trust, and a lack of research, all of which hinder integration into formal healthcare.
Common continental challenges include the absence of standardized regulation, insufficient clinical research, and risks of foreign exploitation of indigenous remedies. Efforts by the World Health Organization (WHO) and African regional bodies underscore the need for formal policies, regulatory frameworks, and collaborative research to ensure safety, efficacy, and equitable benefit-sharing in traditional medicine integration strategies.
Kenya’s current initiatives reflect this broader agenda. A proposed bill in the Kenyan Parliament aims to regulate and integrate traditional medicine by criminalizing false claims, introducing quality control measures, conserving medicinal plants, and requiring biochemical and clinical trials for traditional remedies under the Kenya Medical Research Institute (KEMRI)’s oversight. Kenya already hosts the Centre for Traditional Medicine Research (CTMDR) within KEMRI, which is mandated to carry out scientific evaluation, quality assurance, and clinical research on traditional medicines in collaboration with both local and international partners
Stakeholders, including traditional healers, researchers, and healthcare professionals, have been advocating for greater collaboration and inclusive frameworks that validate and safeguard indigenous knowledge while improving health outcomes. Additionally, Kenya aim to strengthen international partnerships with India ahead of the WHO Traditional Medicine Global Summit held in December 2025, to build capacity on regulation, research, and standards for integrating traditional and complementary medicine into health systems.

Source: 2023 Ministry of Health survey
A 2023 Ministry of Health survey found that nearly 70% of Kenyan households use some form of traditional medicine, often without accurate dosage, clinical trials, or regulation. In rural counties like Kilifi, Kwale, and Tana River, herbal practitioners operate openly, trusted as custodians of indigenous knowledge but often working outside formal oversight. This reliance on unverified treatments has allowed harmful concoctions and misdiagnoses.
In Kenya, 57% of people seek treatment from traditional healers or herbalists compared to 28% who go to health facilities, while 80 % of people in developing countries rely on traditional medicine for primary health care.

A woman and her son fetching water in Kwa Binzaro near Shakahola in Kilifi County. Photo Courtesy Teryani Mwadzaya.
While the scars of Shakahola remain, community resilience, education, and regulatory reforms offer a path toward healing and prevention. The fight for justice is ongoing, but hope persists.
As Kenya confronts the painful legacy of Shakahola and the fresh alarms raised in Kwa Binzaro, the country stands at a crossroads where justice, public health, cultural identity, and state responsibility intersect. The calls from families, healers, researchers, and faith leaders show that preventing another tragedy will require more than arrests or exhumations, as it demands stronger accountability, community education, psychological support, and decisive regulation of both religious and traditional health practices.
With reforms such as the KEMRI Bill and the Quality Healthcare and Patient Safety Bill on the horizon, Kenya now has an opportunity to build a safer, evidence-guided system that honors indigenous knowledge while protecting citizens from exploitation. The challenge ahead is ensuring that the lessons of Shakahola translate into lasting safeguards so that no community is ever again left vulnerable to dangerous doctrines, unregulated remedies, or institutional silence.