
View of Kiberia Slums. Source: Alice Mburu for Andariya Magazine.
That night in June 2020 was extraordinarily quiet as Betha Akinyi strenuously walked to a nearby health facility. There was no loud music playing in pubs, neither was there the constant hooting of matatus - public transport vehicles. The narrow path she took snaking from her home in Gatwikira area in Kibera Slums, about 8 Km from Nairobi city centre, was deserted. It was 3 AM in the morning during Kenya’s nationwide overnight curfew from 7 PM to 5 AM- placed by the government to curb the spread of COVID-19.

Betha Akinyi inside her house in Gatwikira, Kibera slums. Source: Alice Mburu for Andariya Magazine.
Earlier on, Betha (31) who was 8 months pregnant at the time, was woken up by excruciating pain signaling an early onset of labour. “When the pain became unbearable I phoned a traditional birth attendant who lived nearby to come and assist with the delivery,” she recalls. But, the traditional birth attendant was hesitant to assist Betha in the delivery as she had not undergone the necessary routine check-ups conducted during pregnancy. Betha had only attended one antenatal visit, and thus had not undergone most of the required check-ups.
Obstetric Emergencies During the Pandemic
Even though expectant women in informal settlements experienced barriers in accessing quality healthcare well before the pandemic, the COVID -19 crisis has pushed the hurdles to worrying levels.
While the whole country and most parts of the world experienced disruptions in health services during COVID -19, vulnerable populations living in informal settlements have been severely impacted. The pandemic has disrupted maternal, neonatal and child care. The initial months of the pandemic were the worst as the nationwide curfew made it difficult to access clinics at night. “Most women were clueless about what to do in case they experienced labour at night. They would end up enduring and waiting for daybreak to go to hospitals or deliver at home,” says Everlyn Bowa, Founder of (AWOCHE), a health rights community organization based in Kibera.

Evelyn Bowa, Founder of AWOCHE. Source: Alice Mburu for Andariya Magazine.
Health and Socio-economic Fears
This was the case for Betha, her fear of getting infected with the Coronavirus at the hospital made her shun antenatal clinic (ANC) visits. Besides, Betha who sells samosas – a local deep fried pastry- on the streets to earn a living was afraid that if she tested positive for virus she would be quarantined . “As my family’s main provider, I could not fathom the thought of being away from them even for a day,” says the mother of 6. Her husband does menial jobs to earn a living.
Due to fear, many women like Betha did not attend the four ANC visits recommended by the World Health Organization (WHO) during pregnancy. In Kenya only 58% of women make the recommended 4 or more ANC visits during pregnancy according to Kenya Demographic Health Survey KDHS 2014. Adherence to the 4 ANC visits is likely to be higher among wealthier and more educated women. ANC visits from a skilled health provider are important for monitoring the pregnancy to reduce the risk of morbidity and mortality of both mother and child during pregnancy and delivery.
Help in Time of Need
Transport costs and poverty are barriers to accessing maternal health services, contributing to high death figures of mothers during delivery and morbidity in informal settlements. But an innovation by the Kenyan doctor Jemimah Kariuki at the onset of the pandemic has helped bridge this gap for women especially in slums. The solution dubbed Wheels4Life offers free ambulance service for mothers during curfew hours. Patients call a toll free number (1196) and a worker at the call center dispatches a taxi with a movement pass to respond to the emergency.

Shiela Usamba with her 10 months old son at her residence. Source: Alice Mburu for Andariya Magazine.
Sheila Usumba from Darajani, Kibera got to use the service after her labour started at midnight. The onset of labour caught her and her husband by surprise. Sheila quickly made a call to a social worker in Kibera and was amazed when a taxi was sent her way within a few minutes. “The service saved my life. I don’t know what would have happened if they did not respond,” says the mother of a 10 months old baby boy. Since the project was launched in April last year, it has received 120,112 calls and linked 9856 mothers to doctors. Wheels4life has dispatched 1218 cabs and made 855 ambulance trips ,according to data from the Kenya Healthcare Federation (KHF).
In Kibera for instance, the service helped many women access care by qualified personnel during medical emergencies. “During the first months after the launch, we would receive more than 11 calls from expectant women per night,” stated Everlyn who helped coordinate the service. Through partnership between public partners and corporate donors the service is offered free to women who need it.

Shiela Usamba. Source: Alice Mburu for Andariya Magazine.
Ramifications of the Second Wave of the Pandemic
For many women in slums, the effects of COVID-19 disruptions affected more than just their individual well-being, but also the health of their children. Months after giving birth to a healthy baby girl, Betha lost her to pneumonia complications last month. “The child had breathing complications and when we went to the hospital she was diagnosed with pneumonia. The diagnosis was made on a Monday and on Wednesday she was put on oxygen,” she says. With the cost of oxygen being USD 300 per hour, Betha requested that the child be discharged because she had exhausted all her money. Her daughter passed on hours after getting discharged. Betha believes that if the cost of accessing medical care was not so prohibitive, her daughter would still be alive.
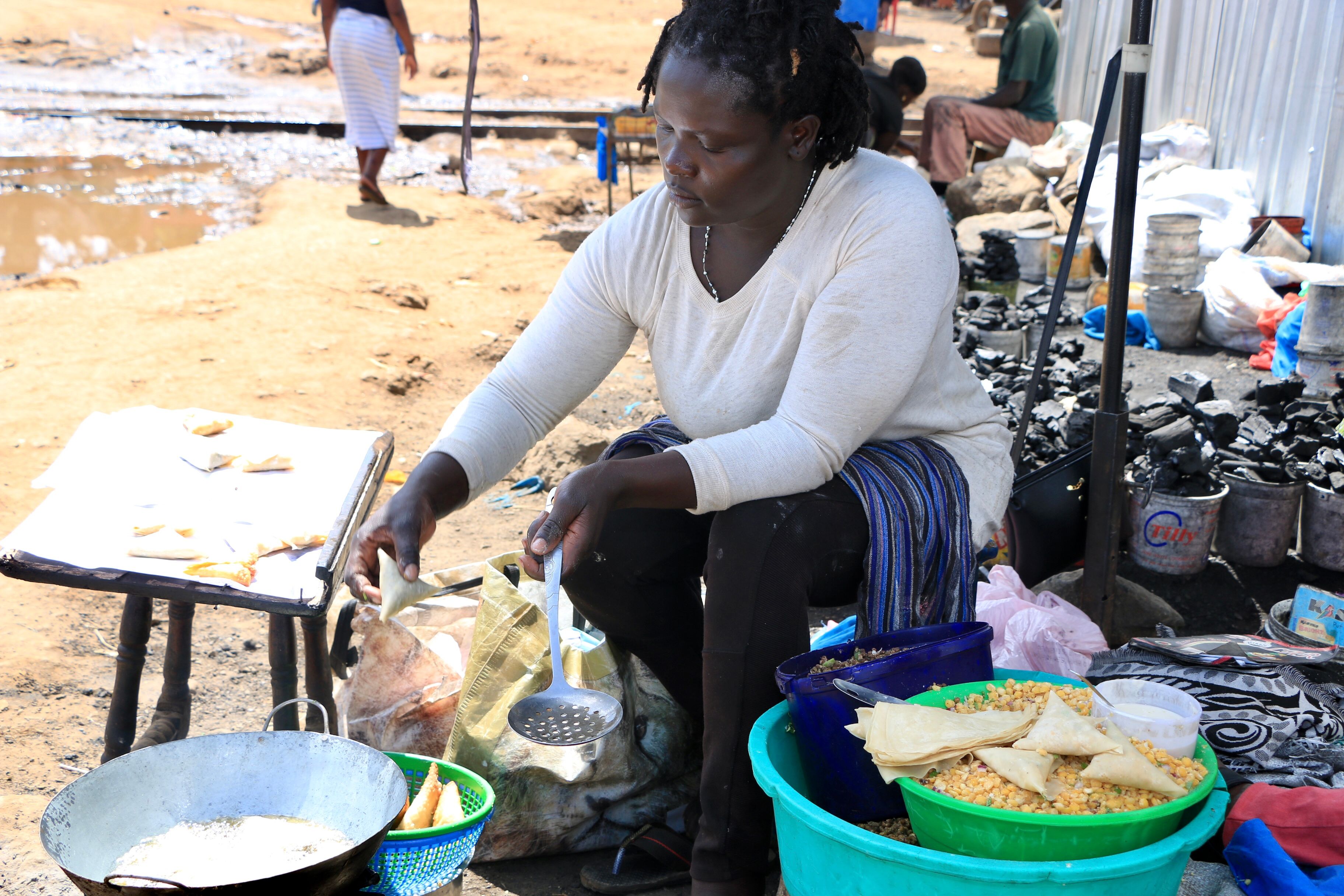
Beth Akinyi making Samosas. Source: Alice Mburu for Andariya Magazine.
Family planning and child immunization services have also been adversely affected. Sheila, recently found out that she is 5 months pregnant after the family planning method she was using failed. The 19 year old who dropped out of school last year after getting pregnant worries that getting a second child will further derail her dream of furthering her education. Living with the father of her child in Kibera with no income has not been easy for her. Sheila is hesitant to visit any health facility for ANC fearing that the health workers will judge her for inadequately spacing her pregnancies. Getting food and other basic necessities is a struggle. I worry about how my second pregnancy will turn out” her voice cracks after a brief pause, as she drifts deep into her thoughts.
*Quick facts about antenatal care (ANC) :
- ANC is essential for protecting the health of women and their unborn children.
- Through ANC women learn healthy behaviors during pregnancy from skilled medical personnel and receive social, emotional and psychological support.
- During ANC women can also receive micro-nutrient supplementation, treatment for hypertension to prevent pre-eclampsia as well as immunization against tetanus.
- ANC can also provide HIV testing and medication to prevent mother to child transmissions.
- Countries in Sub-Saharan Africa have the lowest rate of ANC visits at 13%
Data according to UNICEF.
This article is part of a series on COVID-19's impact in the East Africa region supported by WAN-IFRA Women in News, Social Impact Reporting Initiative.
